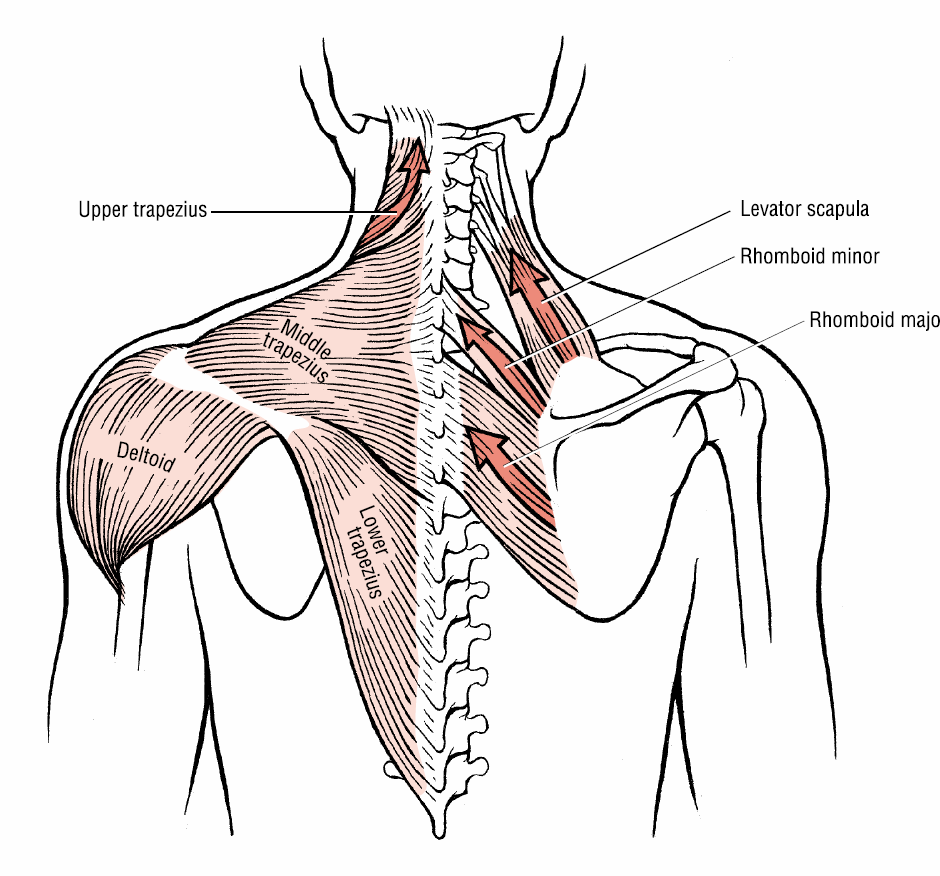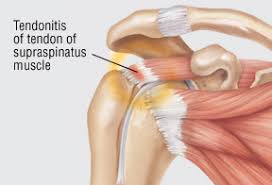
Supraspinatus tendinitis is a common cause of shoulder pain in those people performing overhead activities such as tennis, swimming or baseball. The rotator cuff of the shoulder consists of four muscles; the supraspinatus, infraspinatus, teres minor and supscapularis. The supraspinatus is responsible for abduction, moving the arm away from the body. The supraspinatus muscle may be squeezed by abnormal bony pathology or by inflamed tendons and bursa in the shoulder. The pain of supraspinatus tendinitis is felt in the upper arm. The intensity is moderate to severe. The pain is often felt at night when sleeping on the shoulder. There is pain over the greater tuberosity of the humerus (upper arm bone). The pain worsens when elevating the arm away from the body. As the disease progresses, it becomes more difficult to raise the arm. Testing includes history and physical exam by your doctor. X-rays of the shoulder will look for abnormal bony pathology. CT and MRI scans can look for problems in the rotator cuff and shoulder joint. Initial treatment is conservative and includes heat, ice, physical therapy and non-steroidal anti-inflammatory medications. Injection into the supraspinatus tendon of a local anesthetic and a steroid may both provide a diagnosis and decrease the pain of supraspinatus tendinits.